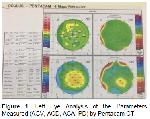
Although leprosy affects multiple organs in the body, the eye is the site where the disease leaves the most sequela
1. The sequela and complications associated with ocular involvement vary depending on a multitude of factors, including the type of leprosy, patients age, genetics, race, and duration of and compliance with therapy. Ocular involvement is commonly seen in leprosy patients
8, and severe complications occur in up to 58% of patients with ocular involvement, leading to irreversible blindness
6. Such patients may suffer from lagophthalmos, ectropion, entropion, ptosis, corneal anesthesia or hypoaesthesia, associated with the involvement of the seventh cranial nerve
9, and this can lead eventually to corneal ulceration and scarring
10, making visual impairment inevitable. A decrease in PD may occur as a result of the involvement of the sympathetic nerve innervating the iris
11, with a mean PD of 3.31±0.42 recorded in the present study. Demir et al.
12 reported a mean PD of 3.57 mm in patients with leprosy. Iris atrophy, chronic iritis and insufficient production of the aqueous humor caused by the involvement of the ciliary body may occur in leprosy patients as a result of the involvement of vascular structures innervating and supplying the iris
13. As a result, changes in IOP are at low levels. In a study by Brand et al., IOP was found to be lower in the leprosy patients who developed chronic iridocyclitis than in the patients in the control group
14. Also in the present study, a decrease was recorded in IOP in the leprosy patients, but this was not statistically significant. Changes to the anterior chamber can occur in leprosy patients as a result of the involvement of the iris and ciliary body. There was a greater decrease in the ACV of the leprosy group than in the control group, but this difference was not significant. That said, ACV and ACA were found to be higher in patients with leprosy when compared to the patients in the control group. A review of literature failed to identify any studies evaluating these parameters in leprosy patients. The authors consider that decreased ACV and increased ACD and ACA in patients with leprosy may probably be due to atrophy of the iris and ciliary body that occurs over time in relation to chronic iritis. Leprosy patients are often rejected by society and abandoned to their fate in an isolated area due to the sequelaon their bodies, particularly those on the face. Accordingly, such patients must be treated promptly without delay upon the diagnosis of the condition. The early application of therapy and follow-up at regular intervals may avoid complications in the ocular structures, where the disease is most often involved
15. There have been studies showing that delays in diagnosis and treatment can lead to blindness associated with ocular involvement
1,5,6. For this reason, the World Health Organization (WHO) launched its 2020 vision program in an attempt to prevent blindness in leprosy patients
16. The present study identified a significant increase in ACD and ACA in leprosy patients, and such changes in ACD and ACA must be taken into consideration when evaluating leprosy patients for glaucoma. There have been different studies evaluating the relationship between glaucoma, and ACD and ACA. In a study of an Asian population, Deverux et al.
17 reported that the anterior chamber depth could play a role when screening for primary angle closure glaucoma. Doğanay et al.
18 found the anterior chamber to be shallower in patients with pseudo exfoliation glaucoma than those in their control group. Another study reported lower anterior chamber volume, depth and angle in patients with primary angle closure glaucoma than in the control group
19. In conclusion, the present study contributes to literature by showing that ocular involvement in leprosy not only produces such sequela as lagophthalmos, ectropion, entropion and ptosis, but can also affect other parameters, such as ACD and ACA. As ocular complications such as cataracts are in leprosy patients
8, subjects from both the patient and control groups were selected from those who underwent cataract surgery, as leprosy patients who have not undergone cataract surgery are rare. The parameters evaluated in the present study may be affected by cataract surgery, which can be considered as a weakness of the study. The authors suggest larger randomized studies be carried out, as the present study involved only a limited number of patients.