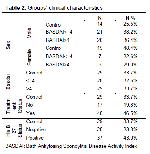
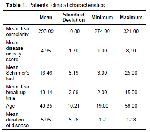
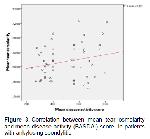
In our study, there were no significant difference in terms of TO, BUT and Schirmers test results between the groups established on the basis of BASDAI, HLA B27 and treatment status with AS.
A decrease in tear production and tear dysfunction on the ocular surface in DES, which develops as a result of various inflammatory diseases, lead to tear hyperosmolarity 16. Tear film hyperosmolarity in turn leads to osmotic stress in the surface epithelium that activates the inflammatory cascade on the ocular surface, and inflammatory mediators are released in the tear 17-19. In 2007, the International Dry Eye Workshop (DEWS) broadened the definition of DES to a multifactorial disease causing increased tear film osmolarity, ocular surface damage accompanied by inflammation, tear film instability and ocular irritability 19. TO measurement is therefore approved by many researchers as a valuable method in the diagnosis of DES, and it has for long been recommended as a potential gold standard in clinical practice 10,20,21.
The prevalence of DES in the normal population ranges between 5.5% and 33.7% 22. Various subjective DES tests have been used in systemic inflammatory diseases in previous studies, such as Schirmers test, BUT, corneal and conjunctival staining, and the ocular surface disease index 23. The sensitivity and specificity of these tests are therefore lower than those of the test measuring TO using the TearLab system. In addition, these tests do not by themselves indicate severity and diagnosis. Definite diagnosis of DES in AS with secondary SS is therefore problematic. To the best of our knowledge, this is the first study to selectively evaluate TO in patients with AS. Additionally, the most important advantage of TO is its ability to reflect the diagnosis and severity of DES more objectively than other measurements 11,20.
One study demonstrated correlations between TO findings and levels of inflammatory mediators in tears 24. The severity of DES may increase in line with the degree of increase in inflammatory activation. We therefore used TO in order to reveal the presence of DES and determine itself severity as a final objective. The TO cut-off value is important for the diagnosis of DES. Cut of values of 305 or 308 mOsm/L have generally been adopted in studies investigating the value of TO in the diagnosis of DES 10,25. In this study we adopted a cut-off value of 305 mOsm/L. This value is sensitive in identifying patients with DES. We identified DES at a level of 12.5% according to TO measurements at low levels of inflammation. The mean age of 40.3 years and low level of inflammatory disease may account for the low level of DES observed.
Markovisky et al. 12 investigated the association between BASDAI levels as a disease activity score for AS and severity of DES using a confocal microscope and various subjective DES tests (OSDI, LIPCOF, Schirmers, and BUT). They observed a significant difference between low and high disease activity levels. All the patients in our study had low inflammation levels (CRP < 0,5 mg/dl), and we used the Schirmers, BUT and TO tests as tests for DES. There was no difference among mild-moderate (BASDAI ≤4), severe (BASDAI >4) and the control groups disease activity levels in the DES tests used. However, we think that if a significant difference can be determined in terms of TO between BASDAI groups in high levels of inflammation, TO can be used as an objective test for disease activity in AS.
Markovisky et al. 12,26 investigated the probable effects of treatment on tear production and LC in patients with AS and rheumatoid arthritis (RA). Although the patients in the group received anti-TNF alpha therapy, that study determined pathology at subjective DES tests and confocal microscopy due to high CRP levels showing systemic inflammatory status. Theoretically, the presence of DES can be explained by increased cytokines in tears in AS with SS with high systemic inflammation impairing tear production.
HLA-B27 is the gene predisposing to primary AS. In a previous study, whereas more than 90% of Caucasian AS patients was found HLA- B27(+), only about 50% of black AS patients was found positive for HLA- B27 27. Furthermore, in another study, The prevalence of HLA-B27 in the white population was stated around 6% to 8%, with HLA- B27-05 being the predominant subtype 28. The function of these molecules is to present antigenic peptides to T cells. They play a significant role in immunological reactions at the cellular level. Laval et al. reported higher relapse, severity and complications of uveitis when they compared HLA-B27-positive patients with HLA-B27-negative 29. In other studies, however, no difference has been determined between HLA-B27-positive and HLA-B27-negative patients either in tests regarding DES or at corneal analyses using confocal microscopy, and HLA B27 has been shown to have no effect on the corneal immune mechanism 4,26. Of the 57 patients with AS in our study, 64.9% were HLA B27-positive. No pathology was determined in either the HLA B27-positive or negative groups in terms of subjective tests as Schirmers and BUT or in more objective dry eye test as TO test.
The main limitation of this study is that TO measurements were performed unilaterally. We performed TO measurements on the right eyes only in all patients due to the limited availability of TO kits.
Conclusions; TO, BUT and Schirmers test results in the groups established on the basis of BASDAI, HLA B27 and treatment status were at normal levels in patients with a low level of systemic inflammation (CRP <0.5 mg/dl). Since AS is an inflammatory disease that progresses with remissions and activations, we think that objective screening of severity of DE using TO can represent a preliminary marker of AS disease activity in association with systemic inflammation level. However, since systemic inflammation levels were low in this study (CRP <0.5 mg/dL), we were unable to prove a relation between TO and disease activity (BASDAI). Further studies may now be planned to establish whether or not TO screening can be used for the definite diagnosis of DES and as a marker of AS disease activity in patients with high levels of systemic inflammation (CRP >0.5 mg/dL).
Acknowledgments
Financial support: No financial support was received for this submission.
Conflict of interest: None of the authors has conflict of interest with this submission