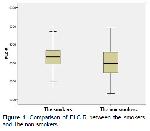
The important findings of our study is that PLC-R was significantly higher in the smokers compared to the non-smokers (Table
1, Figure
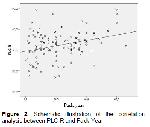
1). In addition, PLC-R and PLCC values have a moderate degree of positive correlation with pack-year (Table
2, Figure
2). There were no statistically significant differences between the two groups in terms of other PVI parameters (Table
1).
Smoking has serious affects on atherosclerosis and promotes coronary artery thrombosis by increasing platelet adherence to endothelium and platelet aggregation 10. It was reported that smoking may increase platelet aggregation and promote endovascular thrombosis through various mechanisms 11. One of the most important mechanism is that platelet survival half-life is shortened by smoking in healthy persons (from 4 days to less than 92 hours) 12. This situation causes to enhancement in reproductibility and aggregability in platelet actions 10.
Larger platelets have more granules and receptors, and prone tend clot more rapidly than smaller ones. Therefore, the platelets activity is more accurately exemplified via their size, not count 13. Platelet size can be evaluated from the PVI, including the PLC-R, MPV, Pct, PDW, PDW/P, and MPV/P 6,14-17.
The MPV is a machine-calculated measurement of the average size of platelets found in blood and is typically included in blood tests as part of the CBC 18. When platelet production is decreased, young platelets become bigger and more active, thus MPV levels increase. Increasing in MPV infers increased platelet diameter, which can be handled as a marker of production rate and platelet activation 19. It is calculated by the following formula, MPV (fL) = [(plateletcrit (%)/platelet count (×109/l)] × 105 20.
The Pct is the ratio of the platelet volume to the whole blood volume (reported as a %) and can be accepted analogous to the hematocrit 20,21. Pct is an effective screening tool for detecting platelet quantitative abnormalities. It is calculated according to the formula Pct = Platelet count × MPV / 10,000 (18, 22-24). Normal platelet count has a Plateletcrit within the range of % 0.22 to % 0.24 19,25.
PLC-R is an indicator of circulating larger platelets (> 12 femtoliter: fL), which is presented as percentage and calculated according to the formula PLC-R = Large platelet cell counts(>12 FL) / Total platelet counts. It has also been used to monitor platelet activity 26. P-LCC is the number of platelets that are greater than 12 fL. P-LCC is the multiplication of Plt× P-LCR 27.
The platelet distribution width (PDW) is the width of distribution of platelets related to the different sizes produced by these cells (28). Inflation in PDW is an indication for the anisocytosis of platelets. Therefore, PDW is an indicator of volume variability in platelets size 19. PDW is a simple platelet index, which is accepted as a specific marker of platelet activation, since it does not increase during simple platelet swelling 29. Briefly, it was accepted that PDW directly measures variability in platelet size, changes with platelet activation, and reflects the heterogeneity in platelet morphology 25,29. In recent study, although PDW and platelet values were not statistically significant between smokers and non-smokers groups, in the correlation analysis performed within the smokers group, it was observed that the pack-year and platelet values were correlated with a weak level and the PDW values were correlated with a moderate level. We think this situation may be because of some PVI values between the two groups are close to each other due to the fact that many cases included in the smokers group have a very low pack-year amount.
Previous studies demonstrated the inverse relationship between MPV and platelet count in normal populations which suggests the need to interpret MPV and platelet counts as a ratio rather than as independent variables 30-32. In the light of this information, we investigated MPV/P Ratio (Mean platelet volume/Total platelet count ratio), PDW/P Ratio (Platelet distribution width/Total platelet count ratio) and PLR (Total platelet count/Total lymphocyte count ratio) in addition to the PVI.
Chronic cigarette smoking results in a increase in platelet activation 33. The platelet function can be detecteded easily by PVI which does not require advanced or expensive technology 5-7. In the present study, we found elevated PLC-R values in smokers than non-smokers and a moderate degree of positive correlation observed between PDW, PLC-R, PLCC values and pack-year. Additionally, a weak but significant correlation observed between platelet counts and pack-year. Possible explanation for why smoking leads to increment in some PVI may be related to chemicals such as carbon monoxide and nicotine in cigarette smoke, which increase platelet activity 34.
The present study showed that smoking is associated with a statistically significant increase in WBC (White blood cell), hemoglobin, hematocrit and triglycerides. On the other hand, lipid profile analysis (total cholesterol, and LDL-C ) in our study, did not significantly different between two groups and this finding is inappropriate with previous findings that showed higher serum levels of total cholesterol, and LDL-C concentrations in smokers 35. There isnt any difference between smokers and nonsmokers with regard to hyperlipidemic cases included in our study and this situation may be responsible for lipid profile results. Secondly, this may be due to dietary differences between the two groups. Last, triglycerides and HDL-C analysis in our study groups were significantly different between the two groups. These findings are consistent with previous findings that showed higher serum levels of triglyceride concentrations and lower plasma concentrations of HDL-C in smokers 35-37.
The harmful effects of cigarette smoking with regard to arterial cardiovascular diseases are well known 38. Plausible mechanisms by which smoking can increase the risk of stroke and heart disease are numerous and include carboxyhaemoglobinemia, increased platelet aggregability, increased fibrinogen levels, reduced HDL-cholesterol 39. Larger platelets are haemostatically more active and are a risk factor for developing coronary thrombosis 40. Some PVI values we observed coincide with the previous research conducted on cigarettes and support the thesis of that healthy smokers are prone to arterial thrombus formation 3,10,33,34,41.
Previous studies have reported that platelet activation increases with age 42. It has also been shown that age is associated with an increase in platelet aggregability 43. Recent studies reported platelet counts and some PVI are positively correlated with obesity as well 44-46. On the other hand, some authors declared refuting findings on these areas 47-48. In our study, participants whose BMI>30 kg/m2 were excluded and there were no statistically significant differences between the smokers and non-smokers group in terms of age. That is why, analyzing of the study results focused on just smoking. The present study revealed that PLC-R is significantly higher in the smokers group compared to the non-smokers group (Table 1, Figure 1, Figure 2). Furtheremore, although there were no statistically significant differences between the two groups with regard to PDW, PLCC (Platelet large cell count), total platelet counts and there were a positive correlation between pack-year and these parameters in addition to PLC-R values (Table 2, Figure 2). Therefore, it is reasonable to say elevated PLC-R level may be a useful indicator of coagulation activity in the smokers.
Conclusions: PVI are important, simple, effortless, and cost effective tools that should be used for predicting the possibility of impending acute thrombotic events. Cases with larger platelets can easily be identified during routine complete blood count analysis and could possibly benefit from preventive treatment. Therefore, more attention should be paid to these indices in the examinaton of a smoker case.