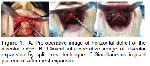
The present study assessed the treatment success rate of implant therapy using two prosthetic restoration types among 19 patients who underwent simultaneous implant surgery with the split crest technique in the maxillary region. The study showed a greater marginal bone loss in patients who were rehabilitated with implant-supported overdentures than those who were rehabilitated with implant-supported fixed prostheses. However, the two groups achieved similar clinical outcomes with respect to prosthetic complications, implant failure, and implant success rate.
In atrophic jaws, particularly in the case of inadequacies in buccolingual direction, the volume of the jawbone should be augmented in order to perform implant therapy. Various techniques such as autogenous onlay bone grafts, guided bone regeneration, and alveolar distraction osteogenesis may be used for repair of the horizontally resorbed alveolar region. Disadvantages of the above mentioned techniques have led to the development of the split crest technique as an alternative 3,4,7. The split technique, a satisfactory procedure among crest expansion techniques, allows for horizontal expansion but no vertical expansion 17. As vertical bone volume augmentation was not needed, the split crest technique was preferred providing expansion in horizontal direction.
In the split crest technique many different materials can be utilized for the splitting; these materials include piezo surgery, sharp osteotomes, ultra-thin fissure drills, and a surgical scalpel 5,6. The most significant risk of the split crest technique is the fracture of the labial cortex 1. Therefore, it requires careful surgery. To ensure the thin alveolar bone would not break at the split region, a mid-crestal starting osteotomy was performed with a scalpel with blade no 15 and the split procedure was completed using thin osteotomes as necessary.
The implant procedure can be carried out in a single stage simultaneously with the split crest technique or in two stages as a staged procedure in the maxilla 1,5,18. Although it is simple to provide primary implant stability and optimum implant positions with the two-stage technique, the treatment duration is prolonged and there is greater surgical trauma. However, with the single-stage procedure there is difficulty providing primary stability and optimal implant position, but it has the advantages of lesser trauma and a shortened total treatment duration 5. The implants were inserted simultaneously with the split crest technique owing to the decent upper jaw supply and the advantages provided by the single-stage procedure.
The split crest technique, including the implant surgery where osteotomized bone segments are formed, can reportedly utilize many materials such as autogenous, allogenous, heterogenous, and alloplastic graft materials alone or in combination 4,19. Likewise, the current study used allograft materials and an autogenous graft combined to fill inter-segment spaces.
Former studies have utilized both periapical and panoramic radiograms to determine marginal bone loss 2,5,6,20. As a single patient received multiple implants in our study, a digital panoramic radiography was used to assess the relationship of the implants with adjacent structures and teeth and to quantify marginal bone loss both during implant planning and follow-up periods.
The amount of marginal bone around dental implants plays an important role in implant therapy 21. Albanese et al.22 reported a mean neck resorption of 1.19 mm during a one-year period after implant therapy using the split crest technique while Gherke et al.5 reported a corresponding figure of 1.76 mm at the end of five months. Furthermore, Filho et al.2 reported that bone loss amounted to 0.47 mm in six months and reached 1.93 mm in 10 years. However, a systematic review reported a marginal bone loss amounting to 0.81.9 mm among patients that underwent the split technique 19. In the current study, like previous studies, the mean amount of marginal bone loss was found to be 1.45 mm. However, that loss was 0.82 mm in Group 1 but 2.14 mm in Group 2. The amount of marginal bone loss was significantly greater in Group 2, which rehabilitated with removable prostheses (overdenture), than in Group 1, which rehabilitated with fixed prostheses (P<0.05). This may have been due to a greater rate of prosthetic complications in Group 2 compared to Group 1 in our study, where patients with prosthetic complications also had a greater marginal bone loss.
Various studies have examined the implant survival rate to determine treatment success after the split crest technique. Those studies have reported implant survival rates of 94%98% 2,5,22. Similarly, two systematic reviews have found an implant survival rate as high as 97% after the split crest technique 4,23. In line with the literature, we found an implant survival rate of 95%. However, this rate was 88.8% and 100% for Group 2 and Group 1, respectively, with both groups being statistically similar with regard to implant failure (P>0.05).
Goodacre et al. 24 reported the complication rate associated with implant-supported overdenture prostheses was greater than implant-supported fixed prostheses. Nedir et al.13 followed 236 patients for eight years and, similar to Goodacre et al. 24, found the complication rate was greater with implant-supported overdenture prostheses (60%) compared to implant-supported fixed prostheses (11%). Bilhan et al. 25, on the other hand, reported no significant difference between the complication rates of removable and fixed prostheses. Also in the current study, the complication rate with fixed prostheses (10%) was found to be smaller than that associated with removable prostheses (44.4%), but that difference did not reach statistical significance (P>0.05). This may due to the low number of patients in our study. At the same time, an increased prosthetic complication rate in the removable prosthesis group led to a lower implant success rate. Similarly, certain other studies have shown that the problems arising with implant-supported overdenture prostheses are mainly related to retainer clips, acrylic resin, or artificial tooth fracture whereas veneer-porcelain fracture and screw loosening occurred more commonly with implant-supported fixed prostheses 11,15,24,26. Similar to the above mentioned studies, the current study revealed a greater amount of retention loss and abutment screw loosening with implant-supported overdenture prostheses, while one patient that received a fixed prosthesis experienced a veneer-porcelain fracture.
In the literature, although increasing age is accepted as one of the risk factors for success of dental implant treatment, the specific nature of the disease process, such as osteoporosis, decreased vascularity, mostly related to aging, are more decisive factor for the success 27,28. In the present study, patients with systemic disorders that would be associated with higher risk of implant failure were not included. The results of this study revealed that the age factor did not cause significant correlations with marginal bone resorption for both groups (P>0.05).
In conclusion, the split crest technique may be used as an effective bone expansion procedure for implant installation in suitable cases with alveolar atrophy in the horizontal direction. On the other hand, the marginal bone loss around the implants was higher in the implant-supported removable prostheses than the fixed prostheses when implant insertion is performed with the split crest technique. However, both prosthetic restoration types yielded similar clinical outcomes with regard to implant survival rate, implant success, and prosthetic complications. Among patients receiving implant-supported removable prostheses, the amount of marginal bone loss may increase over time potentially leading to a greater rate of clinical failure. This study has limitations which potentially affect its findings, including a small sample size and a short follow-up period. Hence, studies with a larger sample size and longer follow-up time are needed to compare different prosthetic restoration types and surgical techniques.
Acknowledgement
The authors thank Professor Tamer TUZUNER for his valuable assistance with the statistical analysis.
Conflict of Interest
We declare that we have no conflict of interest.