Acute lenfoblastic leukemia is an important component of hematopoietic system malignancy that effect young population. Since 1860 Liebreich's first described the leukemic retinopathy form, it has shown that almost all ocular structures were invaded in acute and chronic leukemia
1,2. Ophthalmopathy is common in leukemia especially during periods of active disease in clinical and hematological period6. In postmortem autopsy studies, ocular involvement was found in 82% of acute leukemias and in 75% of chronic leukemia
3. This ratio alters between 9-90% on clinical series
2. Many findings were reported such as infiltration of choroid, leukemic retinopathy, leukemic cells in the anterior chamber and orbital involvement in patients with leukemia
2.
Involvement of eye and adnexia in patients with leukemia may be in a variety such as secondary hemorrhage and infarctions due to anemia or hiperviscosity6.
Although some patients are symptomatic with respect to ocular findings, the majority of patients are asymptomatic. Ocular symptoms of leukemia are decreased visual acuity, leukemic cell infiltration of vitreous and sudden unilateral loss of vision6.
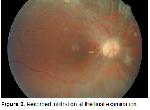
In patients of leukemia, the most common relevant ocular tissue is retina. One of the first findings on fundoscopic examination is dilatation and tortuosity of the veins. Depending on decreased red cell count and increased white cell count, more yellowish appearance in both arteries and veins and retinal vascular sheathing can be seen6. Retinal hemorrhages can be seen at every level of the retina. In addition, it was white centred hemorrhage and it included leukemic cells and debris, fibrin, platelet aggregates. Less common retinal findings like capillary microaneurysms7, peripheral retinal neovascularization8,9 and leukemic epitheliopathy tend to be peripherally located. Another finding in leukemia is retinal cotton wool spots. Ischemia may be caused by anemia, hyperviscosity or leukemic infiltration6,10,11.
Microaneurysms in leukemia may be due to an elevated white blood cell count, in some cases leukocytosis and microaneurysms has not been determined. Increased blood viscosity due to an increased number of white blood cells leads to neovascular activity response and blockage of the terminal arterioles. This is thought to be responsible for the peripheral retinal neovascularization12.
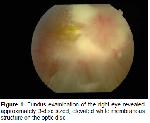
As a result of leukemia treatment, survival rate has increased in recent years. Therefore the CNS involvement is more common3,12. Optic nerve involvement may be a diffuse involvement due to CNS invasion. CNS is infiltrated and inracranial pressure (ICP) increases and causes papilledema. Direct infiltration of leukemic cells in the optic nerve can be seen without intra cranial pressure elevation3. Eye findings of CNS involvement of leukemia can lead to diplopia, blurred vision, or involvement of extraoculer muscle and papilledema, Nikaido et al. reported optic nerve invasion in acute leukemia 13%12. Optic nerve involvement is often associated with CNS or bone marrow involvement in relapses. First relapse may be in the optic nerve when the patient was in remission4. With total remission retinal findings were cured and vision was increased in our case.
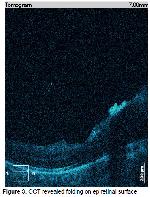
Leukemic infiltration in the OCT findings provides unique images. In our case, OCT findings were consistent with retinal invasion.
As a result, acute relapse may be seen in retina initially. With increased treatment modalities, ocular involvement is becoming increasingly common; with prompt treatment salvage is possible