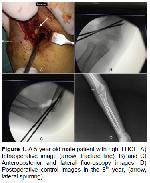
The most commonly cited classification system for pediatric lateral condyle fractures use anatomic configuration (Milch) and displacement (Jacob and Finnbogason) for descriptive and prognostic purposes
3. However, trochlear ossification occurs in children 910 years old and the actual fracture configuration and ultimate displacement cannot be predicted at this age
9. For this reason, the fracture displacement cannot be sufficiently evaluated by standard radiography especially in children younger than 8 years of age
10. Song et al.
11 determined that the internal oblique radiography is more valuable in LHCF. In addition, alternative imaging methods may be used for determining the displacement amount and stability, and MRI provides detailed images for evaluation of the growth plate and cartilage bridge. However, the disadvantages of this method include the necessity of anaesthesia and the high cost
12. Marzo et al.
13 have used arthrography to evaluate the fracture character and displacement range. However, the routine usage of this method is limited. Moreover, ultrasonography may be also used to distinguish stable from unstable fractures
14, the reliability of this method depending on the users experience. Chapman et al.
15 used multi-detector computed tomography to determine the fractures character. The disadvantage of this method is children are subjected to extra radiation. In this study, the varus stress test was applied gently under sedation, the amount of displacement was evaluated under an C-arm fluoroscopy and the treatment method was based on this examination. Existing classification systems are sometimes deemed inadequate in determining treatment modalities and predicting clinical outcomes
3. The effect of the fracture type according to Jacobs classification on functional and radiological outcomes were investigated. There was no statistically significant difference between the fracture types when comparing the functional results according to the Dhillon criteria
8 in each type of fracture.
A very limited number of radiographic criteria have been defined to evaluate a potential displacement and the necessity of an internal fixation during the follow-up of fractures of less than 2 mm 16. Although some orthopedists advocate conservative treatment for minimally displaced (<2 mm) fractures, others suggest open surgical treatment for these cases 17. Among the 51 LHCFs with a displacement less than 2 mm non-operatively treated by Pirker et al. 16, five patients had developed a displacement within the first week as assessed at follow-up visit, suggesting the requirement for an extensive follow-up for non-displaced fractures treated non-operatively.
Surgical fixations are recommended for LHCF treatment involving a displacement over 2 mm. Among surgical techniques related to LHCF, good results are reported between 79% and 96% in various studies, and postoperative complications occur in 0% to 32% of cases 3. CRPF could potentially prevent these complications, even in cases of fractures devoid of cartilage continuity 3. Song et al. 18 have treated lateral condyle fractures with an average displacement of 13 mm and rotation using the CRPF method, and obtained successful results in all 18 patients.
Lateral spurring is a significant radiological finding seen in children followed-up for LHCF 19. Pribaz et al. 19 observed that lateral spur had occurred at different degrees in 73% of their 212 patients treated with different methods. They showed that spur development and size are positively correlated with the fracture displacement at diagnosis. In addition, in the same study, spur occurred more often in cases surgically treated than in those non-operatively treated. Lateral spurs developed in 30 (35.7%) of our cases.
There was a significant difference between lateral spur occurrence and initial fracture. This difference was especially significant between type I and type III fractures. However, lateral spur occurrence did not negatively affect our clinical results.
Cubitus varus is another complication of LHCF 20. Previous studies have shown that the cubitus varus deformity is not related with the treatment method 20. This deformity is generally not symptomatic and surgical correction is rarely required 1. A cubitus varus deformity developed in 6 patients (7.1%) in this study, and these patients did not require corrective osteotomy.
The distal humerus fishtail deformity describes an anatomic finding that originates from the osteonecrosis of the humeral trochlea, but may also result from a central physeal arrest. Generally, this deformity does not imply a functional problem 1. No fishtail deformity developed in any of our cases.
Avascular necrosis (AVN) is a less often encountered complication and is likely related to the surgery 1. However, some authors defend that a surgical approach will not cause AVN and the principal causative reason is excessive dissection 21. Kocher (lateral) approach was used in our cases and no AVN developed in any of our cases.
In conclusion, this study demonstrated no significant relationship between initial fracture displacement, fracture type and clinical outcome. However, the amount of initial displacement may partially negatively affect the radiological result, but radiological changes in the lateral condyle fractures usually do not adversely affect the functional outcomes. Good results may be obtained with the appropriate treatment in the lateral condyle fractures. Cases treated non-operatively should be comprehensively followed-up. In the surgical treatment, sufficiency and stability of the reduction are more important than fracture type.