Epithelial tumors characterized by papillary proliferation of pancreatic duct epithelium and mucin production leading to cystic dilatation are called IPMN. IPMNs are 21% to 30% of all cystic pancreatic masses. Most of the lesions (60%) are seen in the male. It occurs mostly in the 6th to 7th decade
5. It is characterized by an increase in mucin cells producing mucus with different degrees of atypia. In the analysis of cyst fluid obtained by aspiration with EUS, increased amylase level is detected. Because they are associated with the pancreatic duct. If CA 19-9, CEA or CA 72.4 levels are increased, this suggests that it contains a malignant component
6.
Since ultrasonography (US) is an easily accessible, inexpensive, and repeatable test, it is often the first preferred imaging method in the evaluation of the pancreas. The pancreas can be imaged with the US in 75-90 % of cases when appropriate techniques and imaging parameters are used 7. Color Doppler US also contributes significantly to the diagnosis. Besides, US Elastography, and the contrast-enhanced US are useful other modalities 8.
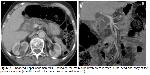
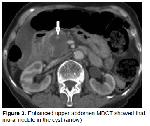
The most important radiological modality in the evaluation of pancreatic pathologies is MDCT. This examination enables high spatial resolution and rapid multiplane imaging in inflammatory and neoplastic diseases of the pancreas. The distinction between normal and pathological pancreatic tissue can often be made safely in contrast-enhanced MDCT. The ductal system is also evaluated. In pancreatic tumors, it is aimed to the evaluation of lesion, arterial and venous system involvement, metastatic changes in the liver and peritoneum, lymph nodes, dilatation that can be observed in the biliary tract and pancreatic duct 9
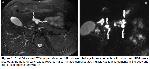
MRI is used as a problem-solving method by imaging pancreatic parenchyma, pancreatic, and biliary anatomy, peripancreatic soft tissues. The addition of sequences such as diffusion-weighted imaging (DWI), MRCP facilitates differential diagnosis of neoplasia and inflammatory processes. The detailed evaluation of both glandular function and pancreatic ducts can be made with the Secretin-stimulated MRCP 10,11. With MRCP, it is possible to detect malignant stenosis of the pancreatic duct and cystic lesions of the pancreas, to characterize and to show the relationship of the cyst with the duct. It is necessary to distinguish the main duct enlargement due to IPMN from the dilatation of the duct caused by chronic pancreatitis. The transition point from the enlarged duct to the normal duct should be evaluated. The main duct in IPMN is progressively thinner without a focal transition point. In chronic pancreatitis, there is a focal stricture at the transition point. Atrophy can be seen around the dilated ductal segment secondary to occlusion and in the pancreatic parenchyma 5,6.
Minor duct IPMNs cause cystic dilation. The main pancreatic duct is normal. They are seen at the head of the pancreas or in the uncinate process (60%) 5. There may be lobulation at the contour and septa in the cyst. It is important to identify their relationship with the main duct in distinguishing it from other cystic lesions in the pancreas 4,5. In the US, the connection of the duct with the main canal cannot be seen. In such cases, MRI and MRCP imaging are required for further evaluation. If present, nodular components or wall thickening may show contrast enhancement after gadolinium injection 5,12. The presence of mural nodules in IPMN is a significant indicator of malignancy. Increased activity can be detected in the cyst wall in IPMNs with high dysplasia in FDG PET-MR 13. Mixed type IPMNs have display features of both main duct IPMNs and minor duct IPMNs 12.
In our study, patients whose main canal diameter was measured ≥10 mm, mural nodules, cyst diameter was measured ≥20 mm, and patients with positive cytology, increased CEA and CA 19-9 values were operated considered as significant risk factors for malignancy. Histopathological diagnosis supported the risk factors of malignancy correlated with the literature 14.
In the literature, the presence of a cyst of ≥30 mm, a positive predictive value is between 25% and 35% for malignancy 15. Also, an increase of more than 2 mm in the cyst diameter during the year, it has been reported that the risk of malignancy development is 45-50 % in 5-year 16.
This study has several limitations. MDCT and MRI images could not be obtained optimally in every patient secondary to respiratory and movement artifact. The main duct and cyst diameter measurements may have a minimal mistake in some patients for this. Cytological examination and tumor markers were not examined in all cases. There were a few patients that did not accept surgery or could not be operated due to additional diseases. So there is a need to research with larger patient series and additional parameters.
In conclusion MDCT, MRI and MRCP are used in the diagnosis and follow-up of IPMN. In selected cases, EUS can also be used for follow-up. Routine follow-up is recommended for patients with IPMN without indication of operation. Cyst size is important in follow-up if there is no risk factor. In the first year 6-month follow-up is sufficient 17. A 6-month follow-up is recommended for patients with relative risk factors for surgery, the elderly and those with severe comorbidity. Also, in patients undergoing partial pancreatectomy for IPMN, follow-up should be done throughout life.