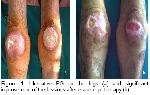
PG is a rare ulcerative skin disease and has been firstly defined by Brocel
2 in 1908 as phagedisme geometrique. Brunstig et al.
11 have proposed the term PG in 1930. PG presents as erythematosus papulopustules or vesicles and gradually shows smooth-bordered ulcers with irregular bases. The ulcers spontaneously either grow or recover after leaving atrophic scars
1-3. It has been reported that 50-70% of the PG cases have an underlying systemic disease
2. The patient presented in this report had not any diseases other than CRF. So far, PG has been reported in 5 cases with overlapping PG and renal diseases [one case as acute renal failure
12, two cases as rapidly progressive glomerulonephritis
13,14 and two cases as CRF
15,16] in the literature (Table
1).

Büyütmek İçin Tıklayın |
Table 1: Summary of pyoderma gangrenosum associated with renal disease reported in the literature |
Pathogenesis of PG is not known in the whole2, but the level of IL-8, a potent chemotactic agent, elevates in PG cases17. TNF-α is a proinflammatory cytokine, which induces the production of IL-8, nevertheless there is no study related to the role of TNF-α in the pathogenesis of PG.
Management of PG initiates by dealing with the underlying disease and primary targets are diminishing pain, helping re-epithelization and finally minimizing the lesion and scar diameters18. Although systemic corticosteroids are popular and the first-line agents in the treatment of PG some of the cases are resistant to this therapy. Additionally, corticosteroids are used in high doses and with long periods of time for the treatment of PG and they can also lead to severe side effects. Immunosuppressive agents, such as cyclosporine, cyclophosphamide, methotrexate and tacrolimus are alternative agents for the treatment in the cases resistant to corticosteroids1-3. Cyclosporine which is effective fairly is administered orally or intralesionally18. However, the use of cyclosporine is restricted due to the facts of nephrotoxicity in oral usage and severe pain in intralesional usage. Hepatotoxicity, myelosuppression, infection and malignancy might be the potential harmful effects of the other immunosuppressives. Although corticosteroids and conventional immunosuppressives take important places in PG management, their effects may be variable18,19. In addition, there is no acceptable treatment guideline for PG.
Infliximab, etanercept and adalimumab the anti TNF-α agents are successfully used in the treatments of rheumatoid arthritis and spondilarthropathies. Anti-TNF therapy has been firstly used by Tan et al.20 in PG and is reported as to be effective. In the following years, anti-TNF agents have been used in approximately 90 cases with PG [some of them are shown in the Table 2 6-9,19-37. Infliximab which has been administrated to 13 PG cases associated with inflammatory bowel disease completely recovered skin lesions in all of them35. In three cases, single dose treatment has provided healing35. In a controlled prospective study19, successful results have been obtained with a proportion of 69% by a single dose of infliximab in the treatment of PG. In similar studies, infliximab has been found successfully effective as 80%36 and 100%35 in the scheme of recommended use in clinical practice. Ljung et al.37 have reported complete recovery in 3 cases, partial recovery in 3 and permanent recovery in 2 cases for the treatment of PG associated with Crohn's Disease (CD) by using infliximab. In this study37, fever, abdominal pain and pneumonia developed as side effects of infliximab. Hubbard et al.28 have treated a case of PG with infliximab but they could not continue the treatment due to anaphylaxis. In that case, during follow-up, etanercept has been determined to be ineffective in recurrence that developed later, and healing has been provided in skin lesion by using adalimumab. In a PG case associated with PAPA (pyogenic sterile arthritis, PG and acne) syndrome32, tacrolimus, mycophenolate mofetil, cyclosporine, etanercept and anakinra administrations have been found to be ineffective, and then infliximab supplied an effective treatment.

Büyütmek İçin Tıklayın |
Table 2: Some of the pyoderma gangrenosum reported cases treated with anti-TNF-α agents in the literature |
Etanercept therapy has been reported in 8 cases with PG6-9,28,32 and complete remission has been observed in 5 cases and partial remission in one, during 1-5 months. The remaining two which are associated with PAPA syndrome32 and idiopathic PG28 have not responded to the etanercept therapy. In our case, etanercept was also effective in PG treatment. Although anti-TNF-α agents are not the first-line options, they might be preferred in induction of remission when good responses are not found with conventional treatments and/or severe side effects are observed. Another advantageous of anti-TNF-α agents might be their rapid effectivity in a short time period.
Reversible demyelinating motor neuropathy might also develop on the base of renal failure38. In the literature 6 CIDP cases related to glomerulonephritis are reported as case reports39-44. In the case presented here, we suggest that CIDP is related to CRF, since there is no other provocative disease. In 25% of the cases diagnosed as CIDP, it is reported that the level of TNF-α elevates4. In addition, it has been found that neutralization of TNF-α has a diminishing effect on Schwann cell apoptosis in experimental autoimmune neuropathy45. Anti-TNF-α agents have also been reported to be effective in the management of CIDP10.
Corticosteroids, intraveneous immunoglobulin (IVIg) and plasma exchange are effective treatments in CIPD46. In cases resistant to the above treatments, azathioprine, cyclosporine, methotrexate, cyclophosphamide and interferons might be used46. Nevertheless, it has been reported that complete remission has been obtained in only one of the three cases with CIDP by using above agents in a retrospective study47 and response to the treatments even with the second and the third generation drugs has been observed to be in 66% of the cases48.
The case presented here was determined as resistant to the steroid administration. As the frequency of acute renal failure has been reported to be as 13% in the cases treated with IVIg49, we did not prefer usage of IVIg due to the presence of renal failure in our case, and etanercept was administreted. Chin et al.10 have reported remarkable recovery in three and partial recovery in three cases with CIDP treated with etanercept (25 mg, twice weekly) for 4 to 6 months. They have also reported recovery in functional scoring in contrary to getting worse in sensorial scores and impairment of all the scores in another three patients and no response in their last case10. As a result, they have suggested that etanercept might be used in CIDP cases refractory and/or intolerant to conventional treatments10.
In our case, while PG manifestations have recovered by etanercept treatment, the adequate response for CIDP has not been observed. This inadequate effect might be resulted from the administration of etanercept for a short time period and its low dose because of CRF in this patient.
To our knowledge, the case presented here is the first one in whom PG and CIDP overlapped on the base of CRF. Etanercept, an anti-TNF-α agent, might be useful in the treatment of PG when conventional modalities are inefficient.