Despite all the advances in cardiac surgery, morbidity and mortality after coronary heart surgery is the most important problem. Diffuse coronary artery disease is defined as multiple stenosis in one or more coronary arteries, distal or partial obstruction of the lumen with the atheromatous material, along the entire length of the vessel
6. In case of diffuse coronary artery disease, it is not possible to anastomose the graft by conventional bypass techniques in such region and even if anastomosed it is often impossible to be beneficial at the distal portion. Therefore, more complex should be applied in such cases
7.
The usage of arterial conduits provides prolonged graft patency and reduce re-intervention necessity 8. In the lesions that partially or completely obstruct the vessel lumen and progress along to distal, the removal of atheromatous material, which is called endarterectomy, is one of the techniques that can be applied. Other technique, in cases where the vessel lumen is partially narrowed is patch plasty in which the arteriotomy is extended to the healthy lumen and the graft is spread over this long arteriotomy area and anastomosis with patch plasty. In cases of multiple stenosis, the arteriotomy can be extended from the proximal along the end of the stenosis or strictures and afterwards the graft is anastomosed to this long arteriotomy 9-10.
The frequency of endarterectomy and reconstruction due to diffuse coronary disease varies according to the clinics, and in some centers, 50% of the cases with coronary revascularization are present 11. According to previous studies, endarterectomy increased peri-operative MI and hospital mortality by 2 fold. Results of the studies from the era of vein grafts, endarterectomy had no benefits regarding to myointimal hyperplasia 12. In a study of Livesay et al. 13 3369 patients were randomized in CABG with endarterectomy or conventional surgery. Mortality and peri-operative MI rates were significantly higher in the endarterectomy group (2.6%, 2.6% vs 4.4%, 5.4%; respectively). The benefits or harms of the endarterectomy is still questionable. The histopathological study of the pathologist Roberts et al. 14 on 35 coronary endarterectomy specimen performed by 7 different surgeons in a single center and 7 years period indicated from Texas that intima and media layer were seen together in all of the samples. He told surgeons that the procedure might better be called endomediaectomy rather than endarterectomy, which determined that the wall of the artery also includes the media layer. There is not any consensus whether to perform or avoid from endarterectomy. Contemporary studies were demonstrated that endarterectomy may beneficial and feasible for selected patients in mid-term survival rates and graft patency. Recent mid-term follow-up studies, in patients with advanced atherosclerosis and severe diffuse atheromatous plaque formation, endarterectomy had favorable effects on preserving myocardial viability and precipitated lesser major cardiac adverse events rather than former studies 15. Wang et al. 16 demonstrated poor short term outcomes for high risk patients with diffuse LAD disease that underwent endarterectomy with CABG while long term results are comparable to conventional CABG. The other study noted increase of cerebrovascular events in CABG with endarterectomy when compared to conventional surgery 17.
We performed long onlay-patch anastomosis without endarterectomy because many aspects remain uncertain about endarterectomy, and there is not a clear recommendation. We did not perform endarterectomy to protect the endothelium and preferred onlay-patch anastomosis also being safe and less complex technique of the onlay-patch anastomosis influenced our choice. LAD-LIMA onlay-patch anastomosis was performed to patients because the distal LAD did not allow for conservative anastomosis due to atherosclerosis. After long segment arteriotomy LIMA graft was directly anastomosed to the LAD and we called it onlay-patch anastomosis 18. During the operation, we experienced that onlay-patch anastomosis technique without endarterectomy was performed easier than endarterectomy technique. Therefore, onlay-patch anastomosis without endarterectomy technique may be better than endarterectomy in patients who would lose the chance of surgery due to diffuse atherosclerosis and multıple stenosis. Also, this technique, facilitate blood flow to the septal perforators and diagonal coronary arteries thus, perioperative MI and related death, the most important complication of endarterectomy 13, can be prevented. In our study, one patient (1.7%) died due to perioperative MI. The mortality rate of our patients who underwent onlay-patch anastomosis without endarterectomy were lower than that of endarterectomy 13,15,16.
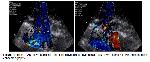
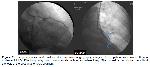
There is some limited evidence to demonstrate microcirculation and blood flow in microvascular bed. CFR measurement after pharmacological vasodilatation is an effective way that supported with studies. CFR values were adequate to estimate hemodynamic significancy at LAD lesions 19. CFR is evaluates the severity of coronary stenosis 20. The determination of CFR by non-invasive method indicates a wide range of pathophysiological conditions, indicating changes in endothelial function in patients with risk factors and in treated patients. Low CFR values (<2) predict epicardial vascular disease associated with microcirculation and multiple cardiovascular, metabolic risk factors may be present 21. In our study, we measured CFR by doppler echocardiography to investigate the presence of epicardial stenosis in patients who had onlay-patch anastomosis without endarterectomy with LIMA after long LAD arteriotomy. As far as we know, investigation of the presence of epicardial stenosis in this long anastomosis line with doppler echocardiography has not been previously described. One of the important results we found; there is a statistically significant inverse correlation between onlay-patch anastomosis length and CFR values (P: 0.008). We evaluated this result as follows; the patch length shows us the presence of intra-coronary lesion that is surgically involved in the more common and longer segment. In such a case, however, the arteriotomy segment is kept longer. More common vascular disease is also compatible with worse coronary microvascular circulation. We think that the cause of lower coronary flow reserve in patients with longer patch anastomosis is due to worse intravascular disease and worse microvascular bed reserve. We performed a more accurate method to confirm graft patency by coronary angiography in a patient with low CFR. In this patient; we believe that CFR is low due to the critical post-anastomotic stenosis.
This study demonstrated the reliability of CFR in detecting graft patency and lower CFR levels are directly associated with impaired viability that represents as decrease in LVEF in echocardiography. Onlay-patch anastomosis technique increases the blood flow in microvascular bed especially in patients with severe diffuse atheromatous plaque at distal vessel. Better results of microcirculation lead to better CFR measurements at LAD flow and directly related with myocardial contraction that presented in echocardiography. It is believed that these results have the clinical strength and meaning to trigger important studies in the near future.
This study had limitations because of restricted and short follow ups that omit long term survival, mortality and graft patency rates. Despite CFR is an accurate and reliable parameter, we could only measure changes in coronary blood flow velocity without coronary artery diameter, but we cannot measure itselves in coronary blood flow. However, it is closely related to the CFR measured using both parameters 22,23. Also, the sample size was relatively small. Randomized cohorts and a control group would increase the statistical power. A long patch plasty with endarterectomy group can be added to demonstrate incontestable results. Finally, coronary angiography was performed in only one patient.
In conclusion, onlay-patch anastomosis without endarterectomy is a relatively safe, feasible and easily applicable technique in patients with severe distal atheromatous plaques. Onlay-patch anastomosis is superior for other conventional methods and more safe than endarterectomy. CFR is a noninvasive and sensitive parameter easily and cost-effectively performed to evaluate bypass grafts.