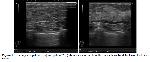
Mastalgia is a very common breast symptom in women attending the breast clinics. It varies within the two broad classifications of cyclic mastalgia and noncyclic mastalgia, cyclic mastalgia accounts for approximately two thirds of patients with mastalgia
8.
Even though many studies done to identify causative histopathological, hormonal, nutritional, or psychiatric abnormalities, few consistent findings have been uncovered, and the etiology of cyclic mastalgia is still unknown.
Increased estrogen, increased prolactin, decreased progesterone levels, or alterations in the estrogen/progesterone ratio are theories regarding the pathophysiology of mastalgia. Menstrual irregularity, oral contraceptives, hormone therapy, psychotropic drugs, some cardiovascular agents (i.e. spironolactone, digoxin), psychosocial factors, and emotional stress are related with breast pain. Caffeine and nicotine consumption are also considered to be related with mastalgia 9,10.
Most women use simple analgesics or get no treatment at all. In rare cases, women with severe pain, persistent pain are treated with drugs; such as danazol and tamoxifen 11. Outcome can be successful in most patients with reassurance, nonpharmacological measures, and in some instances, one of several effective medications 3,12-14.
According to recent studies in the literature, evaluating the psychological associations of cyclic mastalgia, increased anxiety and depression were found among women with breast pain compared to asymptomatic women 6,7,15. As a result of facilitation of access to information by internet, increased awareness, overestimation of breast cancer risk and concerns about cancer prompt more women to seek medical attention and apply clinics more than once for breast pain similar to our patient group.
Our patient group was mostly composed of women with complaints of premenstrual breast pain, tenderness or tender lumpiness and who had increased anxiety and fear about breast cancer. Thus in our study we aimed to evaluate correlation between mastalgia severity and the breast fibroglandular tissue thickness ratio which is primary responsible for the hormonal responses in patients with cyclic mastalgia and to reduce concerns about breast cancer risk by reassurance, as the breast tissue thickness ratio is correlated with mastalgia severity.
While we reviewed the literature we could not find any study evaluating primarily the relationship between with mastalgia and breast tissue thickness. There are few studies identifying a potential association between cyclic mastalgia and breast cancer risk.
Goodwin et al. 16 identified an association of cyclical breast tenderness with breast cancer risk in premenopausal women. They hypothesized that increased tissue sensitivity to estrogen, related to dietary fat intake and fatty acid levels, has an etiologic role in both cyclic breast pain and breast cancer risk and could account for the relationship. Consistent with Goodwin et al. 16 and Plu-Bureau et al. 17 evaluated cyclical mastalgia as a marker of breast cancer susceptibility symptoms in premenopausal women with and without a history of breast cancer and, demonstrated that cyclic mastalgia was significantly associated with breast cancer risk.
Duijim et al. 18 demonstrated prevalence of breast cancer is similar in symptomatic and screening group in their observational 2 year follow up study.
Breast mammographic density, a measure of the extent of radiodense fibroglandular tissue in the breast, can be used as a predictor of breast cancer risk. Breast cancer risk is strongly elevated in women with a high percent mammographic density 19,20. Women with more than 75% of the total area on a mammogram occupied by dense area have a two to sixfold greater risk of breast cancer compared to women with little or no dense area on a mammogram 21,22.
We know that the present study had some limitations. We used VAS scoring system because of high-patient volume in general surgery out-patient clinic instead of any questionnaire specific to breast complaints. In addition we could not follow up of patients for long term.
As a conclusion, in the literature there is no proven obvious association between cyclic mastalgia and breast cancer risk. Thus the primary advantage of breast ultrasonography in women with cyclic mastalgia who do not have a pronounced pathology in their breast sonographies, we can explain it as reducing the pain by relieving the patient psychologically. A more effective analgesic treatment approach and a more careful follow-up in terms of cancer should be applied to patients with high breast density.